 
2 In general, the longer a burn takes to heal, the greater the risk for pathologic scarring. 2 The resulting scar creates an area of skin that is thick, irregularly contoured, stiff, itchy, and painful. Excessively tight collagen bundles, along with absent elastin-for approximately 5 years after a burn-and pro-fibrotic T cells decrease skin malleability. The hallmark is a dysregulation in collagen with the reduced replacement of type III with type I collagen. Hypertrophic scarring is the most common type of scar tissue in a severely burned patient and can be predominantly widespread. High-risk areas for formation include places on the body that experience dynamic tension or areas of naturally tight skin. 5 They can arise after a variety of cutaneous injuries that involve the reticular dermis such as trauma, burns, surgery, skin piercing, and infectious diseases. Hypertrophic scars are those that are raised above the skin level but remain within the original area of skin injury, typically resulting from an overproduction of collagen. 
4 The final phase of maturation and remodeling can continue for years and has the most potential for individual variation in scar qualities.īoth the genetics of a patient and the traits of the tissue play a role in abnormal scarring processes. Epithelialization occurs at this time as well from cell migration over the transitional extracellular matrix. The fibroblasts also stimulate myofibroblasts, which are responsible for wound contraction. The proliferative phase is predominated by collagen and scaffolding molecule formation through activation from deep dermal fibroblasts. Then cytokine reactions initiate recruitment of the major cell types responsible for the restoration of the skin barrier. Stage one lasts for several days where early hemostasis management is achieved through the creation of a fibrin clot. 3 Alteration in any one of these can delay the healing process. The pathogenesis of scar formation progresses in three precise phases: inflammation, proliferation, and remodeling. 2 This management doubles as both a prophylaxis for the development of infection and a means for the reduction of severe scarring. 1 Standard of care surgical efforts to promote healing in deep burns utilize early excision and coverage with split-thickness skin autograft. The patient can then be treated as a typical burn case, with fluid resuscitation and precautions for hypothermia, infection, and rhabdomyolysis. Decontamination can take hours depending on the type of agent and the extent of the injury. Initial treatment involves immediate, low-pressure irrigation of the affected area to completely remove the agent and prevent the spread. Much like more common thermal injuries, this leads to protein destruction and structural changes in the tissue directly contacted by the chemical. Case Overview BackgroundĬhemical burns from acidic agents, as seen in this case, cause damage through coagulation necrosis and cytotoxicity. The authors find these techniques an invaluable part of a reconstructive surgeons' armamentarium when approaching scar revision. This video depicts the combination of both tissue rearrangement techniques as applied to hypertrophic scar contractures resulting from prior burn injuries. Essentially, these techniques illicit a decrease in tension through a lengthening of contracted tissue of up to 50–70%, allowing for better static alignment and increased mobility over joint surfaces. Surgical techniques involving local tissue rearrangement, including Z-plasty and VY-plasty can be employed to improve both the function and cosmetic effects of burn scars. Both sequelae leave the patient with an overall decreased quality of life. 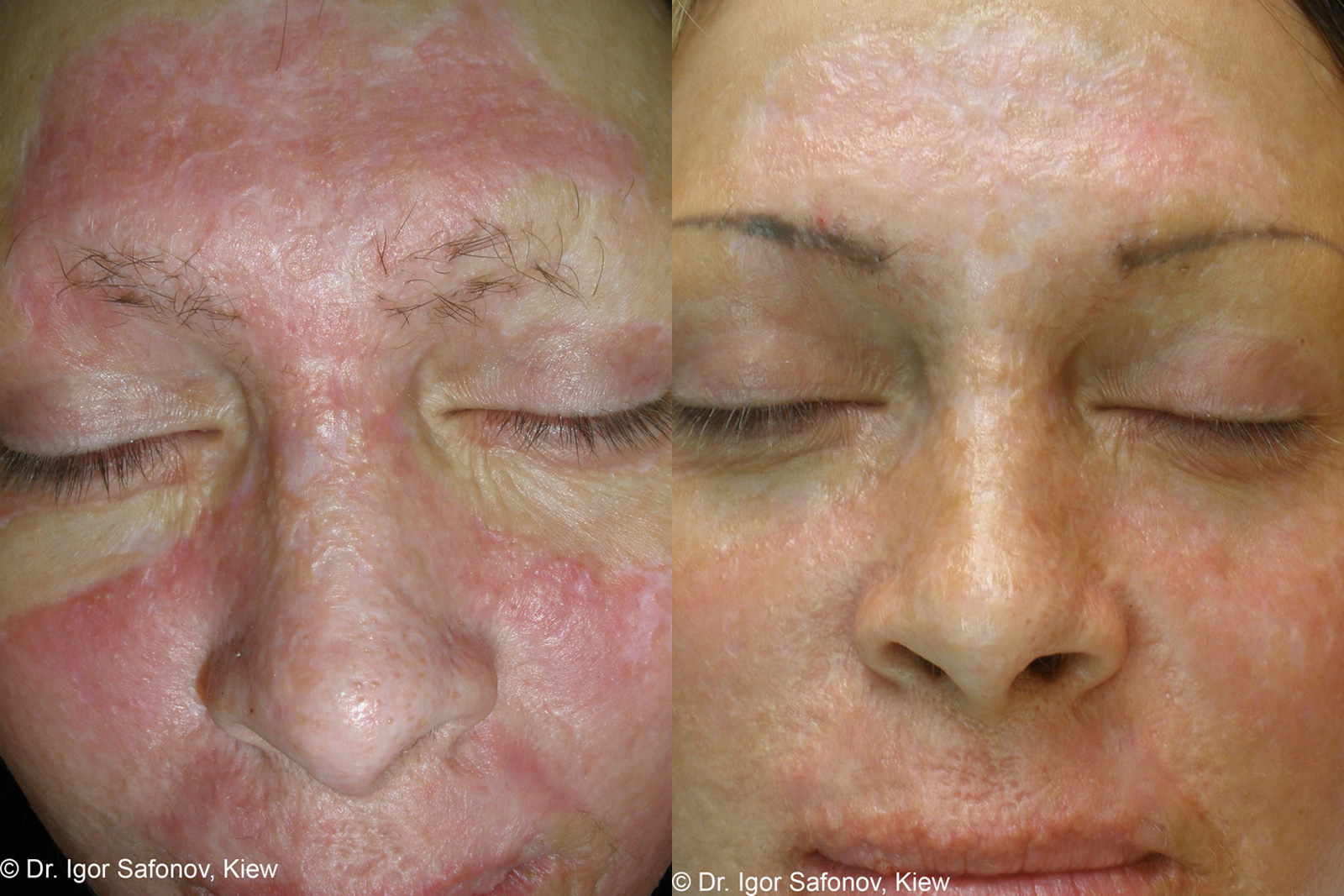
Mobility is jeopardized from contractures that develop within the damaged tissue, leading to decreased range of motion and function of the area. Increased rates of depression and anxiety are seen to arise from aesthetic dissatisfaction, affecting patient rehabilitation and subsequent societal interaction. Hypertrophic scarring following burn injuries has been shown to occur in up to 70% of patients, potentially causing both long-term psychological and physical morbidity.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
